Kidney Health and Diabetes: What’s New in 2026 for Women

Diabetes and kidney health
Diabetes is the leading cause of kidney disease and kidney failure in the United States, yet this serious complication often goes undetected until kidney damage is advanced.
Approximately 20-40% of people with diabetes will develop chronic kidney disease (CKD), and women with diabetes may face additional risks and challenges in keeping their kidneys healthy throughout their lifespans.
The good news is that advances in science and medicine have provided new tools to help women understand their risk of kidney disease and protect their kidneys.
Above-target blood glucose levels cause damage to the small blood vessels that feed the kidneys, impairing the kidneys’ ability to filter out waste products. Damaged kidneys also lose the ability to perform other vital functions, such as regulating blood pressure, keeping bones healthy, and making new red blood cells.
Kidney disease can therefore add to the challenges that women commonly face with bone density and anemia. The risk of developing CKD goes up the longer you live with diabetes.
CKD in women
Women are affected by CKD a little more often than men are.
Changes in hormones in different phases of life can impact blood glucose, increasing the risk of kidney damage. Hormonal changes also affect heart health, which plays a role in kidney function.
Having CKD can affect fertility and pregnancy outcomes. Pregnancy impacts blood glucose levels and can increase stress on the kidneys.
Women are more likely to have urinary tract infections, which can harm the kidneys.
Social factors can also impact kidney outcomes for women. Research suggests that women are sometimes diagnosed later or may be treated differently due to variations in symptoms or healthcare access.
Two important tests for kidney health
CKD does not have obvious physical signs in its early stages.
While foamy urine can be an earlier sign, symptoms like fatigue, swelling, and nausea appear as kidney function gets worse.
Laboratory tests are the best way to identify CKD early. Kidney health is checked with Urine Albumin-to-Creatinine Ratio (UACR) and Glomerular Filtration Rate (eGFR).
- UACR measures how much albumin (a type of protein) is in urine. Albumin in
urine (albuminuria) can be an early sign that the kidneys are under stress.
- eGFR is calculated from the ratio of albumin to creatinine and shows how well the kidneys are filtering waste. An eGFR below 60 for three months or longer may indicate CKD.
GFR is usually included in reports from routine tests, making it easy to track your results. Urine protein can be measured from a single urine collection ordered by your healthcare provider.
Kidney health and the 2026 standards of care
The American Diabetes Association’s 2026 Standards of Care in Diabetes recommend screening for kidney disease early and regularly.
The guidelines recommend that people who have had type 1 diabetes for 5 years or more and all people with type 2 diabetes be checked for both urine protein and GFR at least once a year.
People with diabetes and CKD should be checked 1-4 times per year, depending on the stage of their kidney disease.
The chart below shows the stages of CKD based on the levels of GFR and urine albumin, or albuminuria.
The more serious the damage to the kidneys is, the more often kidney function should be checked. Your healthcare team is most likely to talk about the stages of CKD using numbers 1 through 5.
When CKD reaches stage 3a or 3b, it’s a good time to see a kidney doctor (also called a nephrologist) for specialized care to slow kidney damage.
When CKD reaches stage 5, dialysis or a kidney transplant is needed.
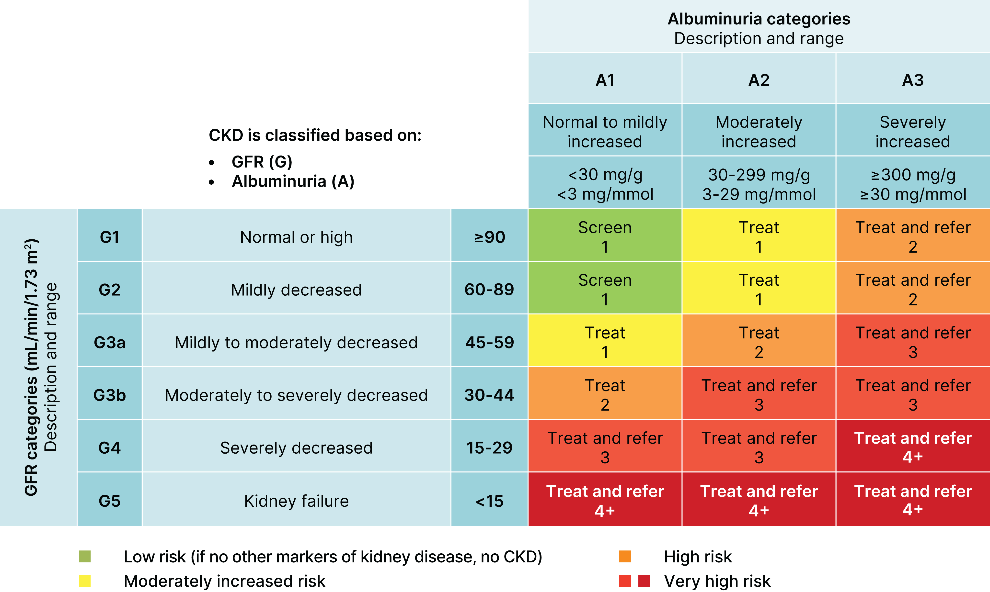
From: 11. Chronic Kidney Disease and Risk Management: Standards of Care in Diabetes—2026
Medical advances are improving CKD outcomes
Some exciting advances in diabetes and CKD include medications that help manage blood glucose AND protect the kidneys from damage related to diabetes. These medicines work in several ways, including helping with blood glucose management, reducing pressure in the kidneys, and lowering inflammation in the body.
Recent studies of a few different types of newer medicines have shown reduced risk of serious kidney and heart problems in people with diabetes and kidney disease.
Examples of newer medicines include semaglutide, dapagliflozin, and finerenone. These medications are most commonly used for people with type 2 diabetes.
Nutrition in managing chronic kidney disease and diabetes
While being on the right medications is important, nutrition can play a big role in kidney health.
The DASH eating pattern has been shown to positively impact kidney health. DASH emphasizes fruits, vegetables, whole grains, healthy fats, and lean sources of protein.
The key is increasing beneficial nutrients like potassium, calcium, magnesium, and dietary fiber, and limiting sodium and saturated fats.
When CKD enters the picture, eating less protein can reduce stress on the kidneys, helping to keep them functioning longer. Better yet, replacing some or all protein foods from animal sources in your eating plan with plant-based foods has been shown to protect kidney function.
A registered dietitian specializing in diabetes and kidney disease can help you develop a personalized eating plan that supports both blood glucose management and kidney health.
If you’re looking for practical guidance to get started, DiabetesSisters offers a helpful resource: Meal Planning Tips for Diabetes and Kidney Disease. This guide includes a 7-day kidney-friendly meal plan, along with tips for balancing nutrients such as sodium, protein, potassium, and phosphorus while still enjoying satisfying meals.
Working with a dietitian can help you adapt meal plans like these to your individual health goals, lab results, and lifestyle.
To find a qualified nutrition professional, the Academy of Nutrition and Dietetics and the National Kidney Foundation both offer online directories that can help you locate registered dietitians who specialize in diabetes and kidney care.
Make yourself and your health a priority
As women, we are often caregivers, juggling the needs of others with our own.
Remember that you are best able to support others you care for when you feel in control of your own health. And remember that you are not alone.
Chronic conditions can be stressful to manage.
Connection and peer support with other women with diabetes can help you navigate diabetes and kidney health management. DiabetesSisters hosts monthly peer-led Meetups and expert-led topic-specific groups to support you in your journey.
If CKD is a part of your personal health journey, kidney health peer support resources, such as the National Kidney Foundation’s PEERS program or KidneyLyfe may provide valuable support and connection.
About the Author:
Rory C. Pace, MPH, RD, CSR, FAND, FNKF, is a Registered Dietitian and a board-certified specialist in renal nutrition, with over 25 years of experience providing care for people with kidney disease. In her current role as Nutrition Therapy Consultant at Patient Care America, Rory supports people on dialysis who are struggling with malnutrition.




