Meal Planning Tips for Diabetes and Kidney Disease

Meal planning looks different for everyone, but this guide can help you get started with meal planning for diabetes and kidney disease. Talk to your healthcare provider about your specific needs. You can also make an appointment with a Registered Dietitian Nutritionist (RDN) to help you make a plan that works for you.
Start with the Diabetes Plate Method
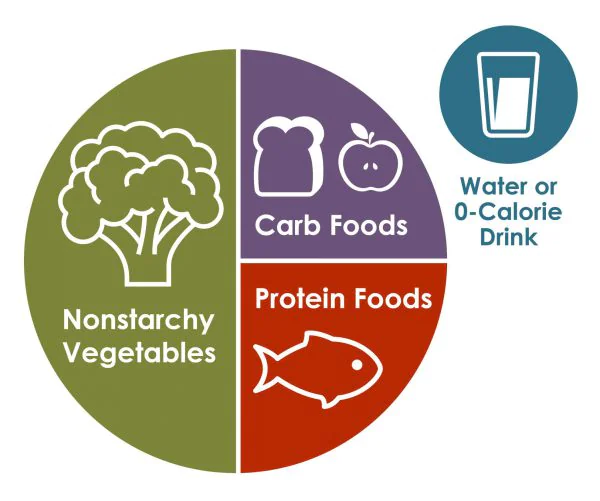
Fill ½ your plate with non-starchy vegetables
Examples:
- Broccoli
- Green beans
- Zucchini
- Bell peppers
- Salad greens
These vegetables provide fiber, vitamins, and minerals while supporting blood glucose management.
Fill ¼ your plate with lean protein (include plant-based options)
Examples:
- Fish
- Chicken
- Tofu
- Eggs
Protein supports muscle health and helps you feel satisfied after meals.
Fill ¼ your plate with higher-fiber carbohydrates
Examples:
- Brown rice
- Quinoa
- Corn
- Whole-grain pasta
Higher-fiber carbohydrates may have less impact on blood glucose levels and can support overall heart health.
Be mindful of sodium
Too much sodium can strain the kidneys and raise blood pressure.
How to check sodium on food labels
Look at the % Daily Value (%DV) next to sodium on the Nutrition Facts label:
- 5% or less = Low in sodium
- 20% or more = High in sodium
Helpful tips:
- Cook with minimal added salt.
- Use herbs and spices instead of salt substitutes (many salt substitutes contain potassium).
- Choose packaged foods labeled “low sodium” when possible.
Choose heart-healthy fats
Healthy fats support cardiovascular health, which is especially important for women living with diabetes.
Choose:
- Olive oil
- Avocados
- Nuts
Also aim for low-calorie or zero-calorie beverages, such as water or unsweetened tea.
How much is too much protein?
Protein needs are based on a person’s weight, and the amount someone with diabetes and kidney disease needs is similar to everyone else, about 0.36 grams per pound of body weight. You can use this online calculator tool.
Protein does not have carbs, but too much animal protein may not be recommended for later stages of kidney disease. Choose plant-based proteins like lentils, chickpeas, tofu, edamame, or black beans.
Common myths and facts about meal planning, diabetes, and kidney disease
Let’s clear up some confusion.
Myth: Whole grains, nuts, seeds, and beans have too much phosphorus.
Fact: Although they contain phosphorus, you don’t need to eliminate them completely. Your body absorbs only about 50% of the phosphorus from unprocessed, plant-based foods. Nuts, seeds, and beans are excellent protein sources, while nuts and seeds also provide healthy fats. Whole grains with higher fiber content are a healthier carb option and may have less impact on blood glucose levels.
Myth: Everyone should follow a low-potassium eating plan.
Fact: A low-potassium eating plan isn’t necessary for everyone. If your blood tests indicate high potassium levels, reducing potassium intake may be recommended. However, if your levels are too low, you may need to consume more potassium-rich foods.
Myth: You must limit fruits and vegetables.
Fact: Even if you need to choose foods lower in potassium, it’s important to still include at least two servings of fruit and three servings of vegetables each day. The carbohydrates from fruits and vegetables remain healthy options, as long as you stick to the recommended serving sizes.
Myth: Salt substitutes are safer than regular salt.
Fact: Many salt substitutes have potassium. Choose salt-free herbs and spices instead.
Myth: Plant-based eating patterns are unsafe.
Fact: Previously, plant-based eating patterns were thought to be harmful to the kidneys, but it is now understood that they are actually beneficial for both diabetes and kidney health.
Myth: There is only one eating pattern for diabetes and kidney disease.
Fact: There is never any “one-size-fits-all” approach to any eating pattern. Since meal planning is confusing, meeting with an RDN is helpful.
You don’t have to figure this out alone
Meal planning is a continuous learning process. It takes practice, adjustments, and and support.
Start small with planning one or two meals each week, and join DiabetesSisters virtual peer-led meetups to share tips and experiences. Community support can make managing diabetes feel more sustainable and less isolating.
Last reviewed February 2026




